Before continuing this article, get our free Local Anesthesia Quiz
Local anesthetics produce anesthesia by inhibiting excitation of nerve endings or by blocking conduction in peripheral nerves. Cocaine, a compound indigenous to the Andes Mountains, West Indies, and Java, was the first anesthetic to be discovered and is the only naturally occurring local anesthetic; all others are synthetically derived. Cocaine was introduced into Europe in the 1800s following its isolation from coca beans. Sigmund Freud, the noted Austrian psychoanalyst, used cocaine on his patients and became addicted through self-experimentation.
Contents:
- Brief overview of structure & mode of action of local anesthetic
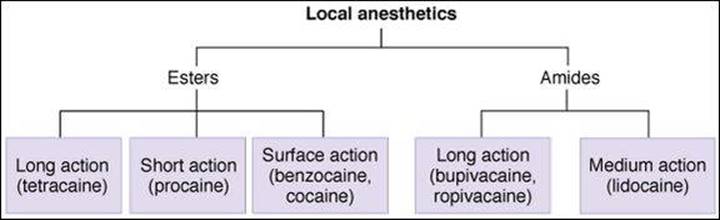
- Different types of local anesthetic
- Safe dosage calculations
- Complications of peripheral nerve blocks
- Treatment of toxicity
- Contraindications
How do local anesthetic work?
Modern local anesthetics are amides supplied in a water soluble weak acid solution
The unionised base diffuses into nerve cells and causes reversible blockade of Na+ channels in excitable neural tissue, preventing action potential propagation
They are less effective in infected tissue due to the relative acidity of the tissue
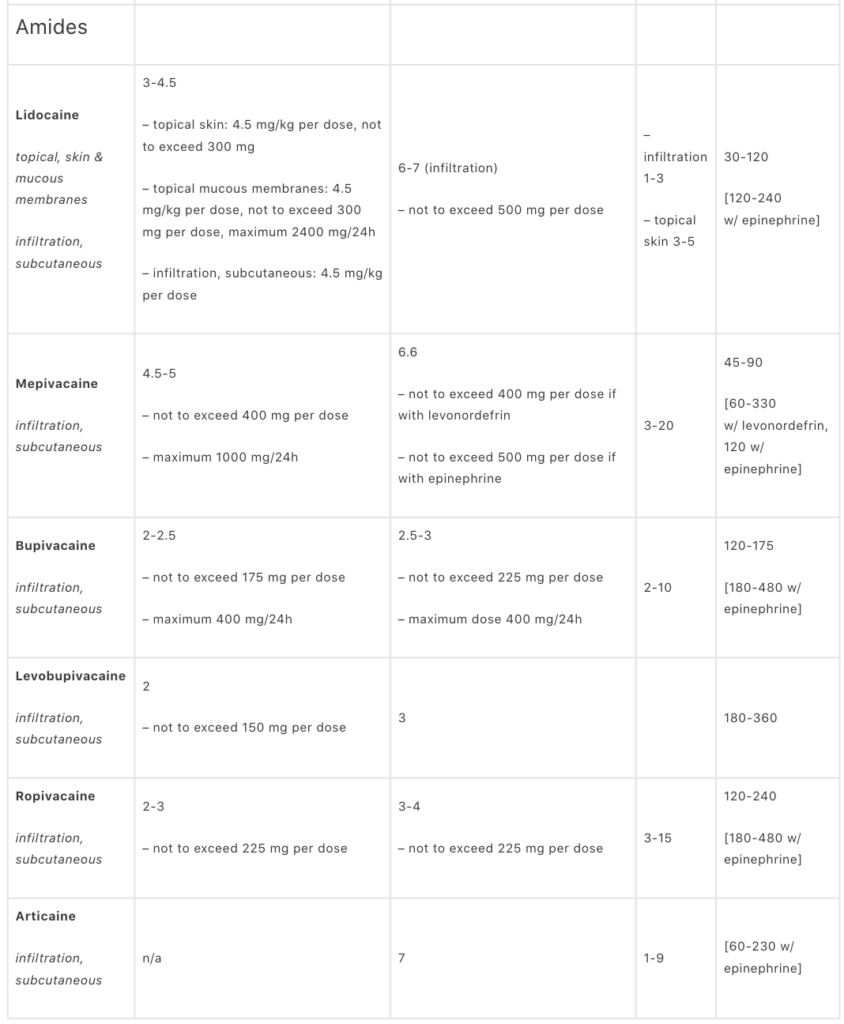
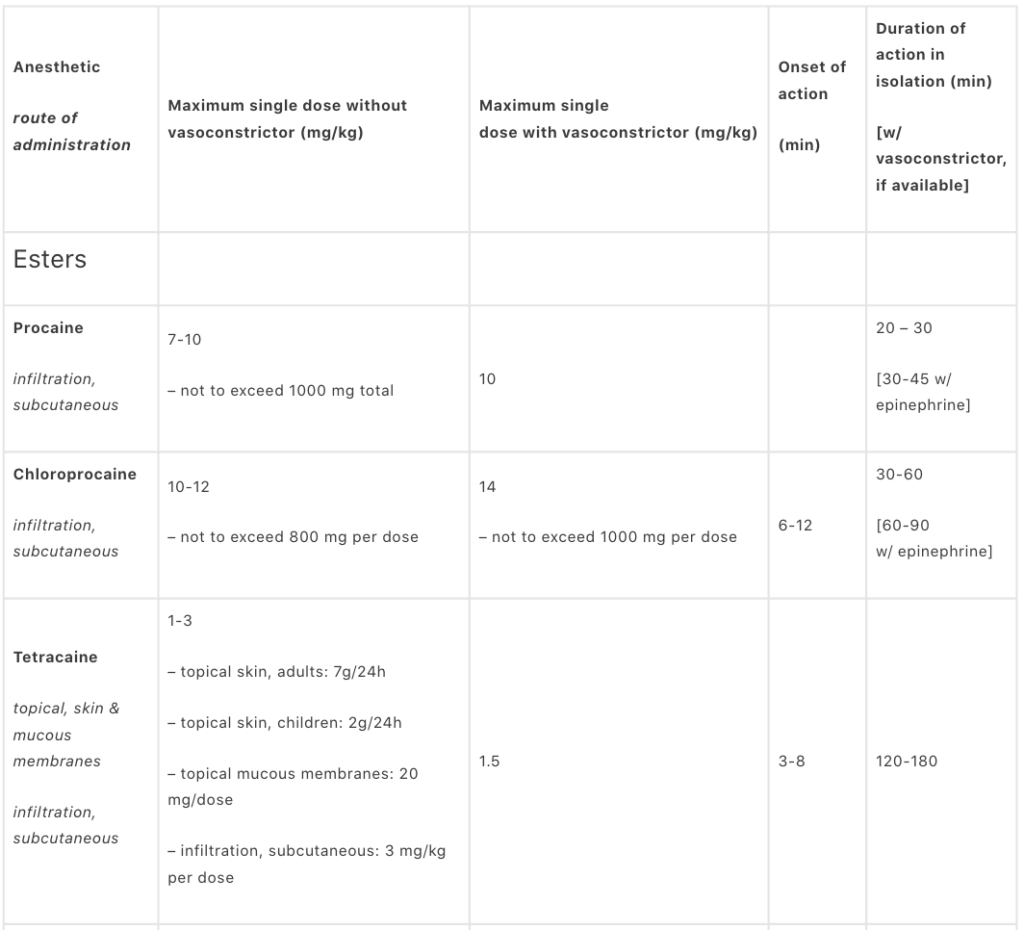
Maximum safe dosages of local anesthetics
- Depends on vascularity of injection site
- Depends on health of patient
- Cautiously increased in presence of adrenaline (vasoconstrictor)
ECG Interpretation and How to Read ECG
Which local anesthetic is better to use?
- Lignocaine (lidocaine)
- Fast onset (< 10 minutes)
- Duration of action 2 hours Max.
- Safe dose: 3 mg/kg
- Cautious dose increase to 5 mg/kg with vasoconstrictor
Local anesthetic dosing for a 70 kg man
- ALWAYS consult the anaesthetist before administration as they may have already performed a regional technique such as a femoral nerve block
The following is a guide for appropriate maximum dosing for lignocaine and bupivacaine Maximum safe dosing
- Lignocaine –
- Max. safe dose = 3 mg/kg – 5 mg/kg if combined with adrenaline
- Available in 1% or 2% solution
- Bupivacaine –
- Max. safe dose = 2mg/kg
- Available in 0.25% or 0.5% solution
Remember: a 1% solution = 10mg/ml and sums are easy!
Calculation of Maximum Recommended Dosage of local anesthetics:
- The concentration of the local anesthetic should be known.
- Percent concentration must be converted to concentration of drug (mg/mL) as follows (table modeled from AAP, AAPD, CJ Cote, S Wilson, Work Group on Sedation)
-
Concentration % mg/mL 4 40 3 30 2.5 25 2 20 1 10 0.5 5 0.25 2.5 0.125 1.25
- The weight of the patient should be known.
Local Anesthetic Examples
1% Lignocaine Example
How much 1% solution can I give to a 70kg man?
- Max. safe dose = 3mg/kg = 210mg
- 1% solution = 10mg/ml so 210/10 = 21ml
- With adrenaline = 5mg/kg – 350mg/10 = 35ml
2% Lignocaine Example
How much 2% solution can I give to a 70kg man?
- Max. safe dose = 3mg/kg = 210mg
- 2% solution = 20mg/ml so 210/20 = 10.5ml
- With adrenaline = 5 mg/kg – 350mg/20 = 17.5 ml
Bupivacaine
How much 0.5 % solution can I give to a 70kg man?
- Max. safe dose is 2mg/kg = 140mg
- 0.5% = 5mg/ml – 140mg/5 = 28ml
Bupivacaine
How much 0.25 % solution can I give to a 70kg man?
- Max. safe dose is 2mg/kg = 140mg
- 0.25% = 2.5mg/ml – 140mg/2.5 = 56ml
More examples about dosage of local anesthetic (Lidocaine):
- Total dose of local anesthetic that can be used
- Maximum dose of lidocaine (plain, without vasoconstrictor) is 4.5 mg/kg (not to exceed 300 mg)
- Example patient weight – 10 kg
- Total dose that can be used for this patient = 4.5 mg/kg x 10 kg = 45 mg
- Maximum volume of lidocaine administered
- Depends on concentration (see conversion table above)
- E.g. for 1% lidocaine: contains 10 mg of lidocaine per 1 mL
- Max volume of 1% lidocaine that can be administered to a 10 kg patient = 45 mg / 10mg/mL = 4.5 mL
ABG interpretation and arterial blood gases analysis
Complications of peripheral nerve block
Technique
- Neural damage
- Bleeding/hematoma
- Intravascular injection of LA
- Infection
- Undesired effects e.g. temporary nerve palsy
Drug
- Toxicity
- Anaphylactoid response (v.rare)
- Methaemaglobinaemia (prilocaine)
Toxicity of local anesthetics
- Immediate: due to intravascular injection
- Delayed: due to absorption from vascular site, accumulation, repeated injection, relative overdose
Systemic toxicity may occur from administration of local anesthetics and is related to the serum concentration of the drug as it is absorbed into the circulation. This serum concentration is influenced by the dose, site, and method of drug administration (Berde & Strichartz, Butterworth et eds, Catterall & Mackie, Curtis et al, Rosenberg et al, Schwartz & Kaufman).
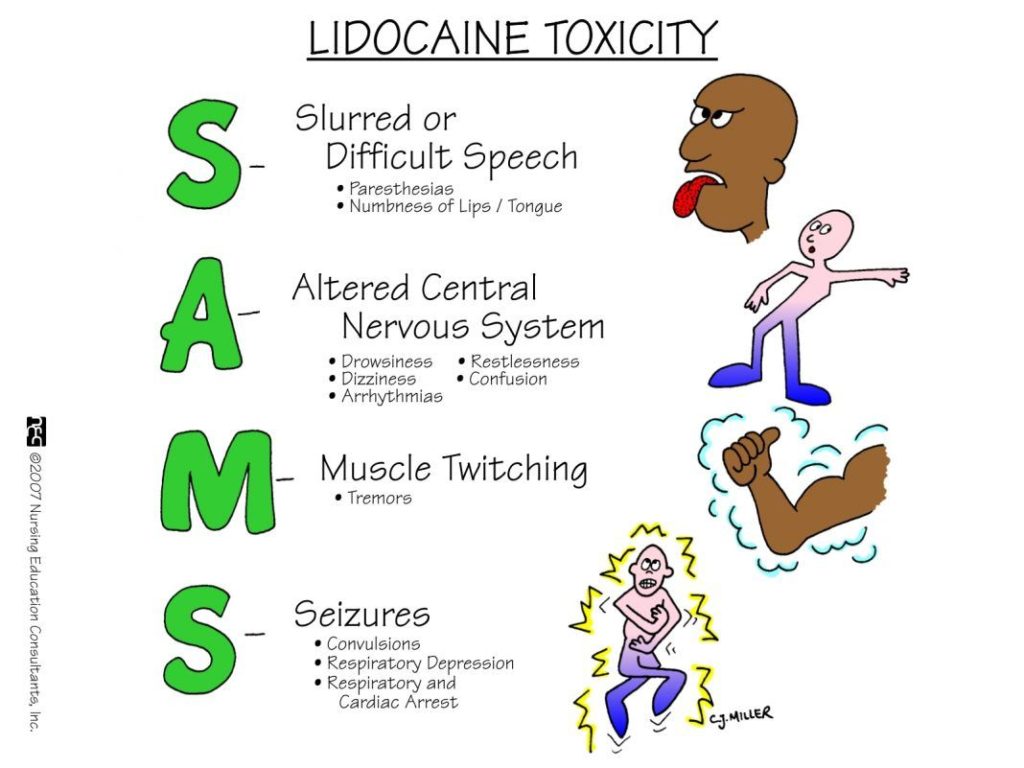
What are the signs of Local Anesthetic toxicity?
- CNS:
- Agitation
- Sleepiness
- Perioral numbness/tingling
- Slurring of speech
- Fitting
- CVS:
- – Hypotension
- – Arrhythmias, often VT/VF
- – Bradycardias ( May be masked by addition of adrenaline to LA)
Management of LA Toxicity
- Call for help
- STOP INJECTING
- Remember A B C
- Administer oxygen, support airway
- Ventilate with bag & mask if necessary
- Ensure iv access, give fluids
- Begin CPR if necessary
Get our free Local Anesthesia Quiz
The only books you need to read about local anesthesia: